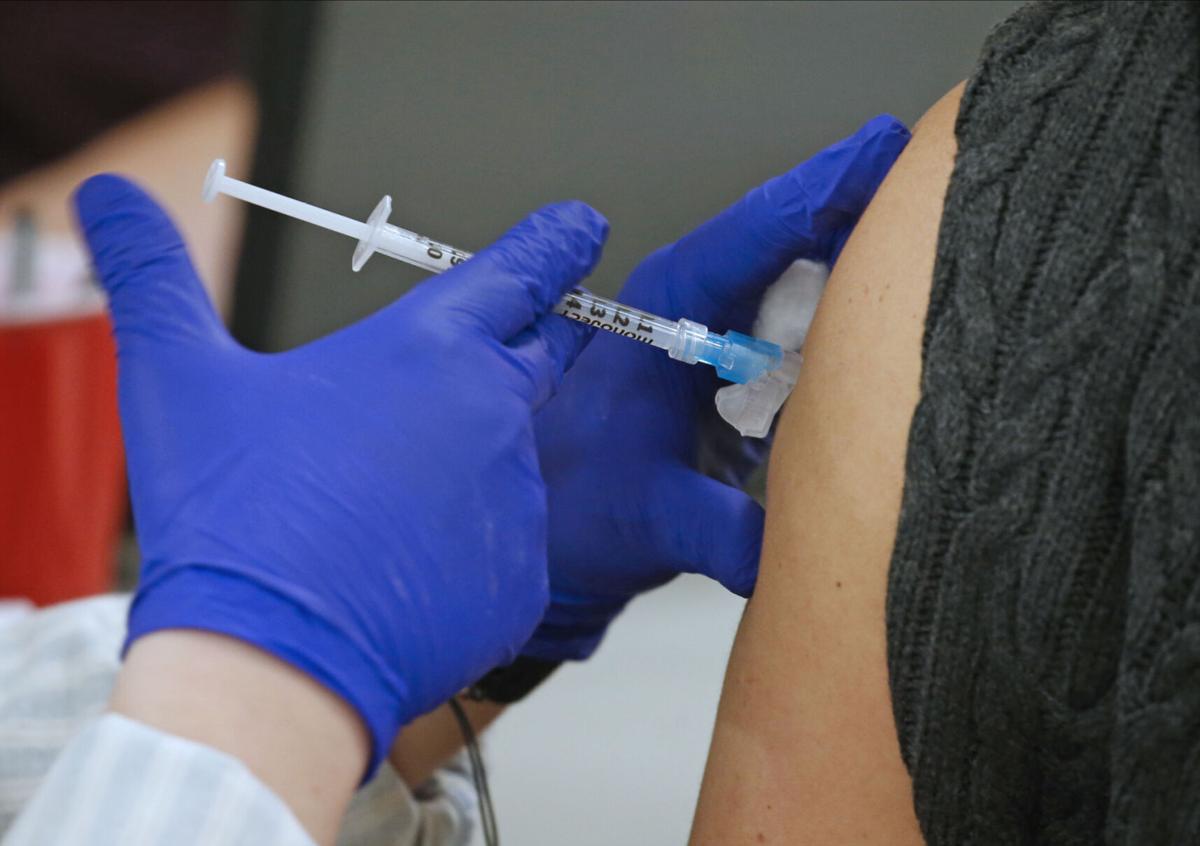
After a single bed-ridden day of fighting off chills and fatigue, Cathy Papia was back to work.
It was a Wednesday afternoon in early January at Buffalo General Medical Center, and Papia was standing in the center of an intensive care unit. Most of the beds were occupied by patients who were unconscious behind glass doors, their bodies deep into a fight against the coronavirus, their gasping lungs silently receiving oxygen with the help of nasal cannulas or ventilators.
“This looks like things are under control, but it’s not,” said Papia, a registered nurse who is the family liaison in the medical intensive care unit at Buffalo General, which – like most area hospitals – is as busy with Covid-19 cases as it was last spring. “People are still dying, and I'm still at the bedside with families sobbing and crying with their dying family members on FaceTime because they can't be there.”
That’s why Papia felt sick the day before. Not because she caught the virus, nor because of the sorrow that constantly surrounds her – that’s a norm now. She was bedridden for the day because she was offered the Pfizer vaccine, and accepted it. Her second dose, which she had received two days earlier on a Monday, evoked an immune response – a sign that the vaccine is working – that had Papia in bed all of Tuesday.
Then she was back – and resolute. “No doubt in my mind, people need to get vaccinated,” she said. “It was a small amount of discomfort to go through.”
In this installment of “Pandemic Lessons,” we speak with medical experts about how to evaluate the pros and cons of vaccination when it is offered to you.
How are we doing so far?
Not everyone is making the same choice as Papia.
Only about 62% of hospital and nursing home workers in Western New York are vaccinated, according to state figures released last week. While the vaccines were recently made available to a larger swath of the public, including front-line workers and people ages 65 and up, it’s difficult to discern broader acceptance rates, since administrative and supply chain issues are causing significant slowdowns.
Epidemiologists say that achieving herd immunity will require up to 80% of the population having some sort of resistance to the virus, which comes from either contracting Covid-19 or getting vaccinated. That six-in-10 figure for healthcare workers provides a clue that achieving herd immunity will be a challenge. It includes not just medical professionals who are heavily steeped in science – doctors, clinical pharmacists, nurses and so on – but also a wider cross-section of people: full-time staff members, assistants and even 17-year-old high school students who work part-time in, say, a nursing home.
On the whole, healthcare workers in hospitals and nursing homes were offered vaccinations first, and on the job — meaning they didn’t have to deal with the frustration of website crashes while making appointments, or with cancellations due to shortage. If they weren’t vaccinated, it was largely because they didn’t want to be – yet. Not because they couldn’t be.
How are clinicians weighing their decisions?
They are analyzing the science – aiming a hard focus at what we do know, and what we don’t – and they are also weighing their social responsibilities.
Multiple medical professionals we interviewed acknowledged the big unknown: “We cannot, with a tremendous amount of confidence, say that there are no long-term side effects to the vaccines,” said Dr. Raymond Cha, a clinical associate professor at the University at Buffalo’s School of Pharmacy and Pharmaceutical Sciences.
That’s because it’s too early to know. What is known, however, is that the first two vaccines, made by Pfizer and Moderna, are about 95% effective. These are the first commercial vaccines to utilize mRNA, a technology that has been in development for years and uses genetic information – not deactivated virus – to stimulate an immune response. Vaccines from Johnson & Johnson and AstraZeneca, which are likely to be submitted for federal approval in the coming weeks and months, use modified adenoviruses, a vaccine approach that has been developed over decades.
Cha, whose pharmacy students have been asking his opinion on whether to get vaccinated, points out the continual advancements in vaccine development as a reason for confidence. “We’re continuing to improve how we’re creating the final product of the vaccines,” he said. “We may not be perfect, but it continues to get better.”
Shouldn’t that qualifier be reason for pause?
Don't expect perfection.
Nothing in medicine is “perfect,” which is why you never hear doctors speak with 100% certainty.
This is where the cost-benefit of vaccination comes into play: We don’t know the long-term effects, if any, of the vaccines. But we do know they were created by scientists who have been developing this technology for years, and who – under the U.S government’s Operation Warp Speed – were able to focus intensely on this single goal, building on years of research, and with many bureaucratic slowdowns presumably removed.
Scientists also don’t know about the long-term effects of Covid-19, for roughly the same reason: There hasn’t been enough time; the illness is just a little over a year old. But there have been early indications that Covid-19 may cause long-term respiratory problems, and researchers are also keeping a close watch on how it impacts the organs.
That presents a difficult but unavoidable choice: Do you get a shot in the arm, and put faith in the skill of the scientists who developed that vaccine? Or do you take your chances, risk catching Covid-19, and hope that the long-term effects of it — whatever they may be – don’t impact you?
And don’t forget: You can die. The death count in Erie County alone exceeds 1,400, while New York is nearing 42,000 statewide and the United States is well above 400,000.
“Perhaps I have the advantage of seeing Covid at its worst, and seeing patients who got exposed” said Dr. Kimberly Zammit, a critical care pharmacist at Buffalo General, who accepted her shot by reasoning it this way: “People get terrible side effects from all vaccines, but they're extremely rare occurrences. In my mind, the potential benefit is that (the vaccine) is going to prevent this Covid disease, and we know what the risk is there.”
Members of the ICU staff at Buffalo General made a practice of talking about the vaccines as information became available. Dr. Manoj Mammen, a pulmonologist, pointed to the “rigorous” review process for the vaccines, as well as the apolitical civil servants and university-affiliated scientists who were involved at the federal and state levels.
“Every time there was a report, I looked into it, I asked my colleagues about it, and it seemed like it was all clarified,” said Mammen, noting there’s also an important social responsibility that supports getting vaccinated. “I hope I’m not the one who gives it to a patient if I’m asymptomatic,” he said, adding two more reasons that apply not only to medical practitioners, but to all: “That I don’t bring it back to my family,” he said, “and that I myself don’t get sick.”
Why not just stay home and wait it out?
You can choose that. And some people– especially those who are immunocompromised – may simply need to shelter as much as possible. But that’s a health problem too. While staying home and avoiding others will lessen your virus exposure, that isolation can lead to a sense of disconnection and disempowerment. That’s particularly difficult now, with both the virus and political rancor ravaging.
For many people, there is “a learned helplessness,” said Dr. Karestan Koenen, a professor of psychiatric epidemiology at the Harvard T.H. Chan School of Public Health, noting that data around anxiety and depression has spiked since last March.
“What can you do but stay in your house?” she said. “It’s this really terrible feeling of helplessness – like your best thing is to do nothing? When there’s a threat, humans were made to do something – fight or flee. And we can’t. We can just sit at home.”
Vaccination – when it becomes available to you – could be your ticket out of that distancing. But it does require you to rely on science – and that’s the inescapable choice.
Note: Do you have a topic or question you’d like to see explored in an upcoming installment of "Pandemic Lessons?” Send it to Tim O’Shei at toshei@buffnews.com or via Twitter (@timoshei).